As a clinical social worker, I have worked with many patients and families who ask why their outpatient treatment is not working. Is it that the psychiatrist/therapist is incompetent? Is their family member simply “not trying hard enough?” Often, the answer to this question is that the symptoms of the person receiving care are too severe for the level of care that they are engaging with.
The problem is that the people with the most information about the patient, the family, do not always know or understand the different levels of care available to help their loved one. Therefore, their experience is one of helplessness and hopelessness.
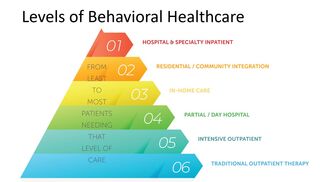 Here, we explore the different levels of psychiatric care available in the United States that may help families navigating these difficult situations. Unfortunately, not all the programs described below are available in every part of the country. We hope this post is a mini "guide" to understanding different levels of mental health care (see diagram).
Here, we explore the different levels of psychiatric care available in the United States that may help families navigating these difficult situations. Unfortunately, not all the programs described below are available in every part of the country. We hope this post is a mini "guide" to understanding different levels of mental health care (see diagram).
Outpatient Level of Care
This is the level of care most people are familiar with. A patient may go see their psychiatrist a few times per month for medication management. The patient may also go see a therapist (for some patients this may be their psychiatrist) once a week or more depending on their symptoms and overall goals. If a person going into outpatient care has severe symptoms, the providers involved may choose to increase the frequency of visits. If this is not effective, it may be time to consider a higher level of care.
Intensive Outpatient Program (IOP)
In general, an IOP is three days out of the week for at least three hours per day. The programs can vary, possibly being more days and more hours. These programs will focus on group work to help the patient develop additional skills to manage their symptoms. The IOP can include medication management services, although not always.
Partial Hospitalization Program (PHP) or “Day Treatment”
These types of programs are five days out of the week for six to eight hours per day. The program will focus on group work and forming a patient community, as well as psychiatric care. A PHP is normally more days than an IOP and will include psychiatric assessment and care. At this point in their care, patients, their families and their providers have identified that treatment needs to be the primary focus rather than work or other family responsibilities.
Community Integration Program/Extended Care
In this level of care, patients are living in a shared therapeutic space with other patients, but the treatment does not happen in the space where the patients live. At Menninger’s Pathfinder Program, residents live in an apartment setting where there is support from resident advisors; however, group therapy and individual therapy happen in a separate location. This type of care allows the patient to maintain a certain level of independence and to focus on increasing their interaction with the community.
Psychiatric Assertive Community Treatment (PACT)
This level of care can best be described as a hospital without walls. In this model of care, one of the primary goals is to keep a person from being hospitalized. It may work well for people who have had multiple hospitalizations in their past and are trying to break that pattern. In PACT, the patients live in their own home/apartment and the clinicians come to the patient, rather than the other way around. Although the PACT model is becoming better known, this is a level of care that is difficult to find outside of major cities.
Residential Level of Care
In this level of care, patients are living in the place where they are receiving treatment. This type of environment can create a safe environment for patients whose functioning is significantly impacted by their symptoms to the point where they are unable to live at home and make progress in their treatment. Resident advisors provide 24-hour monitoring and support.
Sub-acute Hospital Care
This is a level of care that is no longer available in most of the country. In this level of care, a patient is hospitalized for a longer period. At the Menninger Clinic, patients stay in most programs for four to six weeks. There are other psychotherapeutic hospitals where patients might stay with the program for much longer, sometimes years. These types of hospital stays are designed to help the patient stabilize their symptoms but also begin to identify and address some of the more significant core issues that have impacted the person's life. Psychiatric nursing staff provide 24-hour care.
Acute Care Hospital
This level of care offers the highest level of containment. Usually, people who are imminently suicidal or are experiencing acute psychotic/manic symptoms where they pose a safety risk utilize acute hospitalization. The environment is very restrictive as a result. These hospital stays are short, perhaps three to five days. The focus is stabilization and safety. Often, patients and families may feel disappointed in the experience and feel that the core issues were not addressed. An acute hospital stay is not designed to address larger core issues; therefore, outpatient follow-up care is crucial to ensure the best outcome.
A patient can move up the continuum of care as needed, or perhaps they end up in acute care and then move down the continuum as they stabilize. It is important to consider an alternative level of care if a patient is not making progress at their current level of care. If someone feels stuck in their mental health, it would be beneficial for them to look at the level of care they are receiving services at and decide if it is what works best for their needs. It is possible a move in the level of care would dramatically help their mental health.
Note: This content first appeared on Mind Matters from Menninger, our blog on PsychologyToday.com.


